Perioperative 101: A Comprehensive Study Guide
Welcome! This guide details the entire perioperative process, offering essential knowledge for students and professionals navigating surgical patient care effectively.
The perioperative phase encompasses the entire surgical experience for a patient, extending far beyond the actual incision. It’s traditionally divided into three distinct, yet interconnected, stages: preoperative, intraoperative, and postoperative. Understanding this holistic view is crucial for providing optimal patient-centered care.
This phase isn’t merely about preparing for, performing, and recovering from surgery; it’s about minimizing risk, maximizing positive outcomes, and ensuring a smooth transition for the patient through each stage. Effective communication, meticulous planning, and a collaborative team approach are fundamental to success.
We will explore each phase in detail, focusing on the key responsibilities and considerations for all members of the surgical team. This foundational knowledge will empower you to confidently navigate the complexities of perioperative care.
II. Preoperative Phase: Preparation is Key
The preoperative phase is arguably the most critical, laying the groundwork for a successful surgical outcome. This stage focuses on thoroughly preparing the patient – physically, emotionally, and educationally – for their upcoming procedure. A comprehensive assessment is paramount, including a detailed medical history, medication review, and allergy identification.
Verification of physician orders is essential, ensuring all necessary pre-operative tests, consents, and preparations are completed. Patient education plays a vital role, alleviating anxiety and promoting cooperation. Clear explanations of the procedure, potential risks, and post-operative expectations are crucial.
Finally, specific preparations like skin prepping and, when indicated, bowel preparation are undertaken to minimize the risk of infection and optimize surgical conditions.
A. Patient Assessment & History
A thorough patient assessment forms the cornerstone of safe perioperative care. This begins with a detailed medical history, encompassing past illnesses, surgeries, and chronic conditions. A complete medication list – including over-the-counter drugs and supplements – is vital, noting dosages and last administration times.
Allergies must be meticulously documented, specifying the reaction type. Social history, including smoking, alcohol consumption, and drug use, impacts anesthetic and recovery plans. A focused physical examination assesses the patient’s baseline status, identifying potential risks.
Psychosocial assessment evaluates anxiety levels and coping mechanisms. Pre-existing conditions like diabetes or cardiac issues require specialized attention and potential modifications to the surgical plan.
B. Preoperative Orders & Verification
Preoperative orders, typically received from the surgeon and anesthesiologist, dictate essential preparations. These include NPO (nothing by mouth) status, medication adjustments – like holding anticoagulants – and specific diagnostic tests (e;g;, CBC, electrolytes, coagulation studies).
Verification of these orders is crucial. Nurses must confirm completeness, clarity, and appropriateness for the patient’s condition. Any discrepancies or missing information require immediate clarification with the provider.
Order verification extends to allergies, ensuring documented sensitivities align with prescribed medications. Preoperative medications, such as antibiotics or anxiolytics, are administered according to the order. Accurate documentation of all verified orders and administered medications is paramount for patient safety.
C. Patient Education & Consent
Comprehensive patient education is vital before surgery. Explain the procedure, anticipated recovery, potential risks, and alternative treatments in understandable terms. Address patient anxieties and answer all questions thoroughly, fostering trust and reducing fear.
Crucially, verify informed consent. Ensure the patient (or legal guardian) understands the procedure, risks, benefits, and alternatives, and has voluntarily signed the consent form.
Document the education provided, including topics discussed and the patient’s demonstrated understanding. Preoperative teaching should cover pain management strategies, deep breathing exercises, incentive spirometry, and early ambulation. Reinforce NPO guidelines and medication instructions. A well-informed patient is a safer patient.
D. Skin Preparation & Bowel Prep
Skin preparation significantly reduces surgical site infection (SSI) risk. Protocols vary based on surgical site and patient factors; commonly involve cleansing with antiseptic solutions like chlorhexidine gluconate (CHG). Follow facility policy meticulously, ensuring complete application and adequate drying time.
Bowel preparation, if ordered, aims to reduce bacterial load in the colon, particularly for colorectal surgeries. Methods include clear liquid diets, laxatives, and enemas. Monitor electrolyte balance closely, as these preparations can cause dehydration and imbalances.
Document the completion of both skin prep and bowel prep, noting any patient reactions or concerns. Accurate documentation is essential for patient safety and continuity of care.

III. Intraoperative Phase: The Surgical Environment
The operating room demands strict adherence to sterile technique, teamwork, and vigilant monitoring to ensure patient safety during the surgical procedure.
A. Surgical Team Roles & Responsibilities
Effective surgery relies on a coordinated team. The Surgeon leads, performing the procedure, while the Anesthesiologist manages patient physiology – pain, breathing, and vital signs. The Scrub Nurse/Tech maintains the sterile field, anticipating the surgeon’s needs with instruments.
Crucially, the Circulating Nurse coordinates care outside the sterile field, documenting, managing supplies, and advocating for the patient. Each role is interdependent; communication is paramount. Understanding these distinct responsibilities is vital for a safe and efficient operating room environment. Collaboration minimizes errors and optimizes patient outcomes, demanding continuous learning and respect for each team member’s expertise.
Surgeon
The surgeon is the procedural leader, responsible for the surgical intervention itself. This encompasses pre-operative planning, including reviewing patient history and imaging, and making critical decisions during the operation. They directly perform the incision, dissection, and repair of tissues, utilizing specialized surgical techniques.
Post-operatively, the surgeon continues care, monitoring the patient’s progress and managing any surgical complications. Strong anatomical knowledge, precise surgical skills, and decisive judgment are essential. They collaborate closely with the anesthesiologist and surgical team, providing clear direction and ensuring patient safety throughout the entire perioperative period. Ethical considerations and a commitment to optimal patient outcomes are paramount.
Anesthesiologist
The anesthesiologist’s primary role is patient safety during the surgical procedure, achieved through monitoring vital signs and managing pain. Before surgery, they evaluate the patient’s medical history and develop an anesthesia plan – general, regional, or local – tailored to the individual and procedure.
During the operation, they continuously monitor the patient’s physiological state, adjusting anesthesia as needed and responding to any emergent situations. Post-operatively, they oversee the patient’s recovery from anesthesia, managing pain and addressing any respiratory or cardiovascular complications. A deep understanding of pharmacology, physiology, and advanced life support is crucial. Collaboration with the surgeon and nursing staff is vital for optimal patient care.
Scrub Nurse/Tech
The scrub nurse or technician is the surgical technologist, directly assisting the surgeon within the sterile field. Their core responsibility is maintaining a sterile environment and anticipating the surgeon’s needs during the procedure. This includes preparing the operating room, setting up sterile instruments and supplies, and passing those instruments to the surgeon.
Throughout the surgery, they meticulously count instruments, sponges, and needles to prevent retained surgical items. They also manage the surgical field, irrigating and suctioning as directed. A strong understanding of surgical procedures, anatomy, and sterile technique is paramount. Effective communication and teamwork are essential for a smooth and safe operation.
Circulating Nurse
The circulating nurse is the patient advocate and manager of the operating room environment. Unlike the scrub team, they remain outside the sterile field, focusing on patient safety and overall workflow. Responsibilities include verifying patient identity and surgical site, documenting the procedure, and managing supplies and equipment.
They continuously monitor the patient’s physiological status, communicating any changes to the anesthesiologist and surgeon. The circulating nurse also coordinates with other departments, like the lab and radiology, and ensures adherence to hospital policies and procedures. They are a vital link between the sterile and non-sterile worlds, ensuring a safe and efficient surgical experience.
B. Maintaining Aseptic Technique
Aseptic technique is paramount in the operating room to prevent surgical site infections (SSIs). It involves creating and maintaining a sterile field – a zone free of microorganisms. This begins with meticulous hand hygiene and proper attire, including sterile gowns and gloves;
All instruments, drapes, and supplies entering the sterile field must be sterilized. Any break in sterile technique, such as a non-sterile item touching a sterile surface, compromises the field and requires immediate correction. Constant vigilance and adherence to established protocols are crucial. Understanding principles of sterile indicators and maintaining a safe distance are also key components.
Sterile Field Principles
The sterile field represents freedom from all microorganisms, including spores. It’s established prior to the surgical procedure and maintained throughout. Key principles include maintaining sterility only at waist to shoulder level, and considering anything below, above, or to the side of this area as contaminated.
Movement within the sterile field must be deliberate and minimized. Sterile team members face the field, and non-sterile personnel maintain a safe distance. Any doubt about sterility means the item is considered contaminated. Strict adherence to these principles minimizes the risk of SSI and ensures patient safety. Remember, sterility is a state of mind!
Gowning & Gloving
Proper gowning and gloving are fundamental to maintaining the sterile field. Surgical gowns create a barrier between the patient and the surgical team, preventing contamination. Gowning begins with careful hand hygiene, followed by donning the gown, ensuring cuffs cover the wrists.
Closed gloving technique is preferred, maintaining sterility throughout the process. Open gloving requires meticulous attention to avoid contaminating the gloves. Once gloved, team members must be mindful of their movements, avoiding touching non-sterile surfaces. Breaks in sterile technique necessitate regloving or regowning. Consistent practice and adherence to protocol are crucial for patient safety.
Instrument Sterilization
Maintaining instrument sterility is paramount in preventing surgical site infections. Common sterilization methods include steam sterilization (autoclaving), utilizing high pressure and temperature to kill microorganisms. Other methods include gas sterilization (ethylene oxide) for heat-sensitive instruments, and plasma sterilization.
Each instrument must be thoroughly cleaned and inspected before sterilization. Biological indicators, such as spore tests, verify the effectiveness of the sterilization process. Sterile packaging maintains sterility until the instrument is used. Proper storage of sterile instruments is also vital, protecting them from contamination and ensuring their availability when needed. Documentation of sterilization cycles is essential for quality control.

IV. Postoperative Phase: Recovery & Monitoring
Postoperative care focuses on patient stabilization, pain control, wound healing, and vigilant monitoring for potential complications during the recovery period.
A. Immediate Postoperative Care (PACU)
The Post-Anesthesia Care Unit (PACU) is crucial for initial recovery. Upon arrival, a rapid assessment of airway, breathing, and circulation (ABCs) is paramount. Continuous monitoring of vital signs – including heart rate, blood pressure, respiratory rate, and oxygen saturation – is essential.
Pain management begins proactively, utilizing prescribed analgesics and assessing effectiveness. Wound assessment focuses on identifying any immediate bleeding, drainage, or signs of compromise.
Neurological status is frequently evaluated, checking for alertness, orientation, and any deficits. Temperature regulation is also vital, addressing hypothermia commonly experienced post-surgery. Clear communication with the surgical team regarding any concerns is key to optimal patient outcomes in this critical phase.
Vital Sign Monitoring
Consistent and accurate vital sign monitoring is the cornerstone of postoperative care. Blood pressure, assessed invasively or non-invasively, reveals hemodynamic stability. Heart rate variations can indicate pain, hypovolemia, or arrhythmias.
Respiratory rate and oxygen saturation, measured via pulse oximetry, are critical for detecting respiratory depression or compromise. Temperature monitoring identifies potential infection or malignant hyperthermia.
Pain scales, both numerical and behavioral, quantify patient discomfort and guide analgesic administration. Frequent neurological assessments, including level of consciousness and pupillary response, detect potential complications. Documentation of trends, not just individual values, provides a comprehensive picture of the patient’s physiological status, enabling timely intervention.
Pain Management
Effective pain management is paramount for postoperative recovery, influencing patient comfort, mobility, and overall outcomes. A multimodal approach, combining pharmacological and non-pharmacological strategies, is often most successful.
Opioids, non-opioid analgesics (like NSAIDs and acetaminophen), and local anesthetics are commonly utilized, tailored to the patient’s pain intensity and medical history.
Non-pharmacological methods, including positioning, relaxation techniques, and distraction, complement medication. Proactive pain assessment, utilizing validated scales, is crucial.
Careful monitoring for adverse effects, such as respiratory depression or nausea, is essential. Patient education regarding pain control options and expectations empowers self-management and improves satisfaction.
Wound Assessment
Thorough wound assessment is a cornerstone of postoperative care, enabling early detection of complications and guiding appropriate interventions. Assessments should include observation of incision color, edema, approximation, and drainage characteristics.
Documenting the wound’s length, width, and depth provides a baseline for comparison and tracks healing progress. Assess for signs of infection – redness, warmth, purulent drainage, and increased pain.
Palpate the wound edges for firmness or crepitus, indicating potential issues.
Regular assessment, following established protocols, is vital. Accurate documentation facilitates communication among the healthcare team and supports informed decision-making regarding wound care management, including dressing changes and potential need for further evaluation.
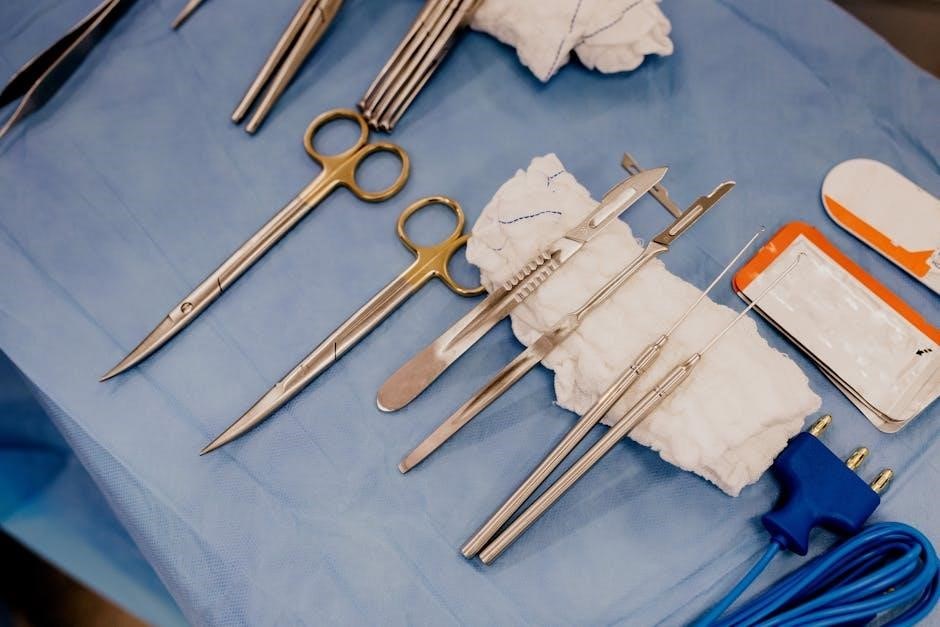
B. Common Postoperative Complications
Postoperative complications, while often manageable, require vigilant monitoring and prompt intervention. Infection, a significant concern, manifests as fever, redness, swelling, and purulent drainage at the surgical site. Bleeding, either internal or external, necessitates immediate assessment and potential transfusion.
Respiratory issues, such as pneumonia or atelectasis, are common, particularly in patients with pre-existing conditions; monitor oxygen saturation and auscultate lung sounds.
Thromboembolic events (DVT/PE) are also risks, requiring prophylactic measures and assessment for calf pain or shortness of breath.
Early recognition and appropriate management of these complications are crucial for optimal patient outcomes.
Infection
Surgical site infections (SSIs) represent a major postoperative complication, impacting patient recovery and increasing healthcare costs. These infections can range from superficial wound infections to deep infections involving tissues, organs, or implanted devices.
Signs and symptoms include localized redness, swelling, warmth, pain, and purulent drainage. Systemic signs, like fever, tachycardia, and leukocytosis, may also be present.
Risk factors include prolonged surgery, contaminated wounds, immunocompromised patients, and poor wound care.
Prevention relies on strict aseptic technique, appropriate antibiotic prophylaxis, and meticulous wound management. Prompt identification and treatment with antibiotics are essential for effective management.

Bleeding

Postoperative hemorrhage is a potentially life-threatening complication requiring immediate attention. Bleeding can occur primarily from the surgical site or secondarily due to coagulopathies. Recognizing early signs is crucial for effective intervention.
Signs and symptoms include excessive drainage from the wound, hematoma formation, decreased blood pressure, increased heart rate, and pallor. Internal bleeding may present with abdominal distension or altered mental status.
Risk factors encompass pre-existing bleeding disorders, anticoagulant medication use, hypothermia, and inadequate hemostasis during surgery.
Management involves direct pressure, application of pressure dressings, fluid resuscitation, and potential blood transfusions. Prompt notification of the surgeon is paramount for possible re-exploration.

Respiratory Issues
Postoperative respiratory complications are common, particularly after abdominal or thoracic surgery. These issues stem from factors like anesthesia, pain, and decreased lung expansion. Early detection and intervention are vital to prevent serious consequences.
Common problems include atelectasis (lung collapse), pneumonia, and hypoxemia (low blood oxygen). Signs include dyspnea (difficulty breathing), cough, decreased oxygen saturation, and abnormal breath sounds like crackles or wheezes.
Risk factors encompass smoking history, obesity, chronic lung disease, and prolonged immobility. Pain can also limit effective coughing and deep breathing.
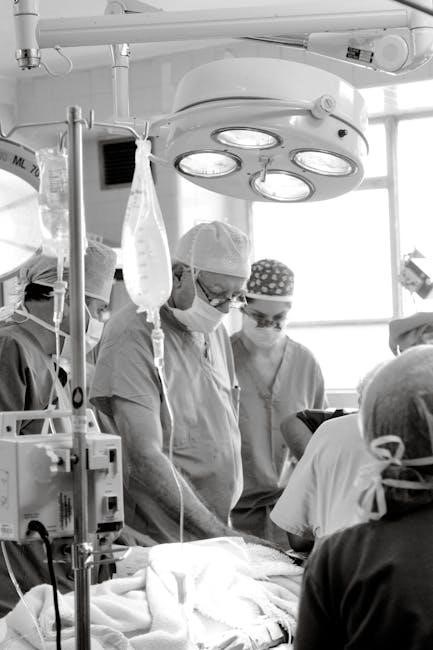
Management focuses on encouraging deep breathing and coughing exercises, incentive spirometry, oxygen therapy, and potentially, respiratory treatments or mechanical ventilation.
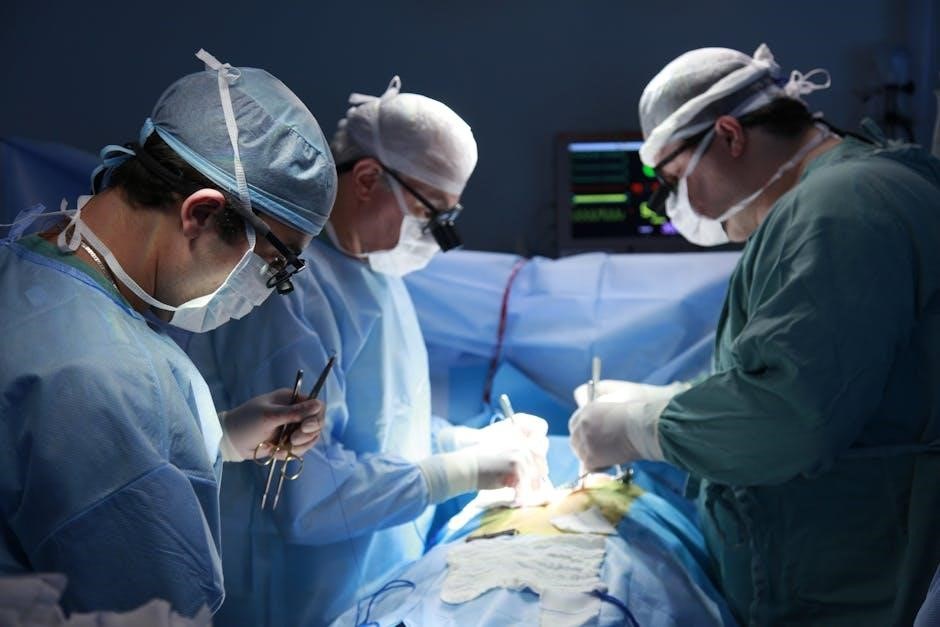
V. Essential Perioperative Documentation
Accurate records are crucial! This section details vital documentation, including checklists, anesthesia records, and detailed postoperative nursing assessments for patient safety.
A. Surgical Safety Checklist
The Surgical Safety Checklist, championed by the World Health Organization (WHO), is a standardized tool designed to enhance patient safety and reduce preventable errors during surgery. It’s implemented in three key phases: before anesthesia, before skin incision, and before the patient leaves the operating room.
Before anesthesia, the checklist confirms patient identity, surgical site, and allergy status. Before incision, it verifies the surgical team has reviewed critical steps, antibiotic prophylaxis is administered, and imaging is correctly displayed. Before the patient leaves, it ensures proper wound counts, labeling of specimens, and addresses any immediate concerns.
Consistent use of this checklist promotes communication, minimizes risks, and fosters a culture of safety within the surgical environment. Thorough documentation of checklist completion is paramount for legal and quality assurance purposes.
B. Anesthesia Record
The Anesthesia Record is a comprehensive legal document meticulously maintained by the anesthesiologist throughout the perioperative period. It details the patient’s medical history, pre-anesthetic assessment, informed consent, and all medications administered – including induction agents, paralytics, analgesics, and fluids.
Crucially, the record documents vital signs monitored during anesthesia (heart rate, blood pressure, oxygen saturation, respiratory rate), any complications encountered, and interventions performed. It also includes the type of anesthesia used (general, regional, local), and the timing of key events.
Accuracy and completeness are vital. The anesthesia record serves as a critical resource for postoperative care, billing, and potential medico-legal review. Electronic anesthesia records are increasingly common, enhancing accessibility and data analysis.
C. Postoperative Nursing Notes
Postoperative nursing notes are a vital component of the patient’s health record, documenting the recovery journey following surgery. These notes detail frequent and thorough assessments, including vital signs, pain levels (using a standardized scale), wound status, and neurological function.
Essential documentation includes intake and output, medication administration (including pain medications and antiemetics), and the patient’s response to treatment. Nurses also record any complications, such as bleeding, infection signs, or respiratory distress, and the interventions implemented.
Clear, concise, and objective charting is paramount. Notes should reflect the patient’s progress towards recovery goals, any patient education provided, and communication with the surgical team. Accurate documentation supports continuity of care and legal defensibility.

VI. Resources & Further Study
For continued learning, the Association of periOperative Registered Nurses (AORN) offers extensive resources, including guidelines, publications, and online courses: https://www.aorn.org/. Explore their evidence-based practice resources for current standards.
Textbooks like “Alexander’s Care of the Patient in Surgery” and “Perioperative Nursing: Principles and Practice” provide comprehensive foundational knowledge. Online platforms like Coursera and Udemy host relevant courses.
Professional certifications, such as the CNOR (Certified Nurse Operating Room), demonstrate expertise. Regularly reviewing surgical journals and attending conferences keeps you updated on advancements. Remember to consult your institution’s policy and procedure manuals for specific protocols and best practices.